Benzos
Benzodiazepines in Australia: Prescribing Patterns and Safety
A brand new way
A Comprehensive Guide for Patients and Healthcare Professionals
Introduction
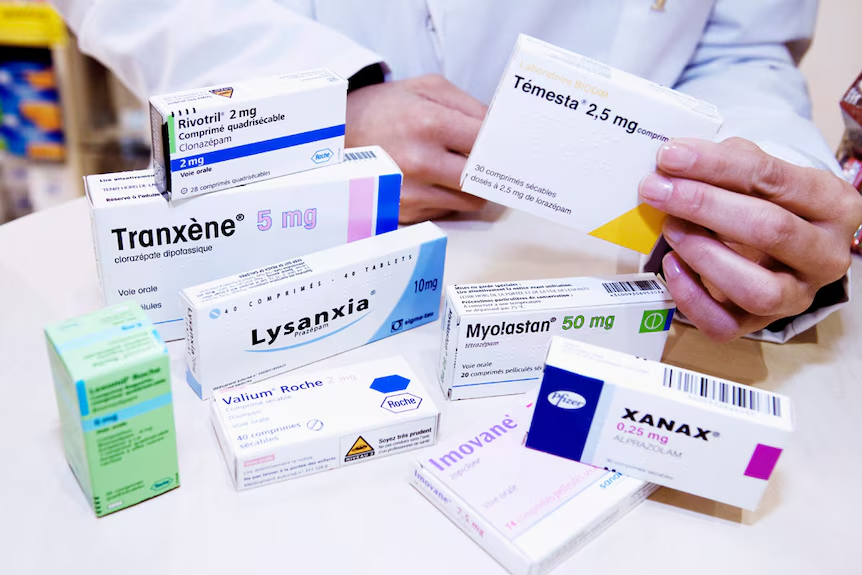
Benzodiazepines remain one of the most commonly prescribed classes of medications in Australia, with 1 in 20 Australians prescribed these drugs annually . Used primarily for anxiety, insomnia, and stress management, medications like Valium (diazepam), Xanax (alprazolam), and Temazepam have become household names. However, recent data reveals concerning trends in prescribing patterns and safety outcomes that every patient and healthcare provider should understand.
This comprehensive guide explores current prescribing patterns in Australia, safety considerations, and evidence-based recommendations for benzodiazepine use.
What Are Benzodiazepines?
Benzodiazepines are prescription medications that act on the central nervous system to produce a calming effect. They work by enhancing the activity of GABA (gamma-aminobutyric acid), a neurotransmitter that inhibits brain activity .
Commonly prescribed benzodiazepines in Australia include :
| Medication | Brand Name | Common Uses |
|---|---|---|
| Diazepam | Valium | Anxiety, muscle spasms, alcohol withdrawal |
| Alprazolam | Xanax | Panic disorders, anxiety |
| Temazepam | Normison, Temaze | Insomnia |
| Oxazepam | Serepax | Anxiety, alcohol withdrawal |
| Clonazepam | Klonopin | Seizures, panic disorders |
| Lorazepam | Ativan | Severe anxiety, pre-operative sedation |
Z-drugs (non-benzodiazepine hypnotics) such as Zolpidem (Stilnox) and Zopiclone (Imovane) are also commonly prescribed for sleep and carry similar risks and precautions .
Current Prescribing Patterns in Australia
Prevalence of Use
Recent data from the Penington Institute reveals that 1.4 million Australians were prescribed 5.1 million benzodiazepine scripts in 2020-21 . This widespread use reflects both the prevalence of anxiety and sleep disorders and the ongoing reliance on pharmaceutical interventions for mental health concerns.
Concurrent Prescribing Concerns
Perhaps most concerning is the practice of concurrent prescribing of benzodiazepines with other central nervous system depressants. A comprehensive study using MedicineInsight data (analyzing records from 1,207,671 patients attending 544 general practices) found that the prevalence of concurrent long-term opioid and benzodiazepine prescribing was 7.0 per 1,000 patients .
Even more alarming, the median duration of prescribing overlap was 611 days far exceeding recommended treatment durations .
Who Is Most Affected?
The same study identified specific population groups with significantly higher rates of concurrent prescribing :
| Population Group | Increased Risk (Adjusted Prevalence Ratio) |
|---|---|
| Smokers | 4.10 times higher |
| Patients aged over 65 years | 3.62 times higher |
| Patients with mental health conditions | 3.23 times higher |
| Socioeconomically disadvantaged | 1.70 times higher |
| Females | 1.33 times higher |
| Rural/remote residents | 1.13 times higher |
Most strikingly, patients with both mental health and musculoskeletal conditions had a prevalence of 32.1 per 1,000 more than four times the average .
Safety Concerns and Adverse Effects
Overdose Statistics
Benzodiazepines are now the second-most common drug involved in accidental overdose deaths in Australia, behind opioids . Key statistics include:
-
544 unintentional drug-induced deaths involved benzodiazepines in 2021
-
The proportion of accidental overdose deaths due to benzodiazepines has doubled in the past 20 years, making up 32.5% of fatalities in 2021
-
Benzodiazepines were involved in 36.7% of all overdose deaths (663 deaths) in 2016
John Ryan, CEO of the Penington Institute, describes benzodiazepines in overdose cases as “always the bridesmaid, never the bride” they are “rarely the single drug in relation to an overdose, but they’re very frequently the companion drug” .
Risks in Elderly Populations
The risks are particularly pronounced in older Australians. A study of 3,064 residents across 23 residential aged care facilities in New South Wales found :
-
40% of residents used at least one potentially inappropriate psychotropic medicine
-
27.4% used benzodiazepines or Z-drugs the most frequently used category
-
Residents with dementia were 1.94 times more likely to use two or more potentially inappropriate medications
-
Prevalence across facilities ranged from 23.3% to 57.0%
The Australian Commission on Safety and Quality in Health Care has launched a new national standard to protect people with cognitive impairment from inappropriate psychotropic use, noting that older people face increased risks of worsening cognition, falls, stroke, and death when prescribed these medications .
Common Side Effects
According to health resource Each, longer-term benzodiazepine use can lead to :
-
Worsening sleep (disruption of REM and deep sleep)
-
Forgetfulness and memory problems
-
Poor coordination and balance (increasing fall risk)
-
Depression
-
Increased anxiety (paradoxical effect)
-
Drowsiness
Drug Interactions
The greatest danger occurs when benzodiazepines are combined with other central nervous system depressants, particularly :
-
Opioids (significantly increased respiratory depression risk)
-
Alcohol
-
Anticonvulsants
-
Antipsychotics
-
Methadone
Dependence and Withdrawal
How Dependence Develops
The Royal Australian College of General Practitioners (RACGP) recommends that benzodiazepines should not be taken regularly for longer than four weeks . When taken regularly beyond this period:
-
The body quickly develops physical dependence
-
Tolerance develops, requiring higher doses for the same effect
-
Withdrawal symptoms emerge when attempting to stop
It is estimated that 4 in every 10 people who take benzodiazepines regularly for more than 6 weeks will experience withdrawal symptoms .
Withdrawal Symptoms
Withdrawal can be severe and potentially dangerous. Common symptoms include :
| Category | Symptoms |
|---|---|
| Psychological | Rebound insomnia, anxiety, panic attacks, perceptual disturbances |
| Physical | Muscle spasms, flu-like symptoms, fatigue, aches and pains |
| Cognitive | Memory problems, difficulty concentrating |
| Gastrointestinal | Nausea, vomiting, diarrhoea |
Important: Patients should never stop benzodiazepines abruptly, as this can trigger severe withdrawal reactions. Dose reduction must be gradual and medically supervised .
RACGP Evidence-Based Guidance
The RACGP provides comprehensive guidance for benzodiazepine prescribing in general practice .
Indications for Use
Benzodiazepines may be appropriate for :
-
Insomnia (short-term only)
-
Anxiety disorders
-
Alcohol withdrawal
-
Mania/hypomania (adjunctive)
-
Epilepsy and acute seizures
-
Arousal/agitation in inpatient settings
-
Palliative care
Management of Insomnia
For acute insomnia, the RACGP recommends :
-
Focus on avoiding or withdrawing the precipitant
-
Basic behavioural counselling on sleep hygiene and stimulus control
-
Short-term benzodiazepines only as an adjuvant for severe, disabling cases
For chronic insomnia, first-line therapy should be non-drug interventions including :
-
Cognitive behavioural therapy (CBT)
-
Brief behavioural therapy
-
Exercise
-
Sleep hygiene education
Key Recommendations
-
Limit duration – Prescribe for no longer than 4 weeks
-
Discuss cessation early – Address dose reduction on first prescription
-
Regular review – Monitor efficacy and adverse effects
-
Avoid concurrent CNS depressants – Especially opioids and alcohol
-
Individualise treatment – Balance risks and benefits based on patient circumstances
Non-Drug Alternatives
Given the risks associated with benzodiazepines, several evidence-based alternatives should be considered :
For Anxiety
-
Cognitive Behavioural Therapy (CBT)
-
Mindfulness and relaxation techniques
-
Selective serotonin reuptake inhibitors (SSRIs) for long-term management
-
Exercise and lifestyle modifications
For Insomnia
-
Sleep hygiene education
-
Stimulus control therapy
-
Sleep restriction therapy
-
Relaxation techniques
-
Brief behavioural therapy (accessible via RACGP’s HANDI resource)